Periodontal Abscess
A periodontal abscess (fig. 5-10) usually results from long-continued irritation by food debris, plaque, deep deposits of calculus, or foreign objects such as a toothbrush bristle or popcorn husk being tightly packed in the interproximal spaces or within the walls of a pocket. The gingiva surrounding the area becomes inflamed and swollen.
PERICORONITIS
Pericoronitis is an inflammation of the gingiva around a partially erupted tooth. The mandibular third molars are most often affected, although any erupting tooth may be involved. In the mouth of a young adult, part of a tooth can be seen projecting through the gingiva, usually distal to the second molar. The surrounding tissues are usually acutely inflamed. The inflammation may be caused by irritation resulting from the patient's inability to keep the area properly cleansed. Another cause of inflammation is infection from oral pathogens that gained access to the tissues surrounding the crown of the erupting tooth through the opening made by a projecting tooth cusp. The "gingival flap" may become infected after inflammation as a result of the constant irritation caused by contact with the occlusal surface of an erupting maxillary third molar.
DISEASES OF THE ORAL SOFT TISSUES
Many oral diseases can affect the soft tissues. We will cover only a small portion of the most common types. These lesions can be caused by viruses, bacteria, fungi, and physical and chemical agents. Direct contact with the diseases covered may present some degree of hazard or a life-threatening disease to you, the Dental Assistant. Always follow infection control procedures when in contact with all patients.
RECURRENT APHTHOUS STOMATITIS
Recurrent aphthous stomatitis (RAS) (fig. 5-11), or canker sores, are painful ulcerations. These lesions
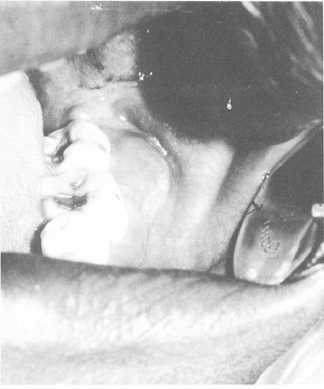
Figure 5-10.- Periodontal abscess.
Continue Reading